Medical Dressings: Classification, Applications, and Usage Methods are essential medical supplies used to cover wounds, protect injured tissues, and create a favorable environment for wound healing. They play a crucial role in preventing infection, absorbing exudate, and promoting tissue regeneration. With the advancement of medical technology, the types of medical dressings have become increasingly diverse, each designed to meet specific wound care needs. This article will elaborate on the classification, applications, and standard usage methods of medical dressings.
Classification of Medical Dressings
Medical dressings can be categorized into several types based on their materials, structures, and functions. The main classifications are as follows:
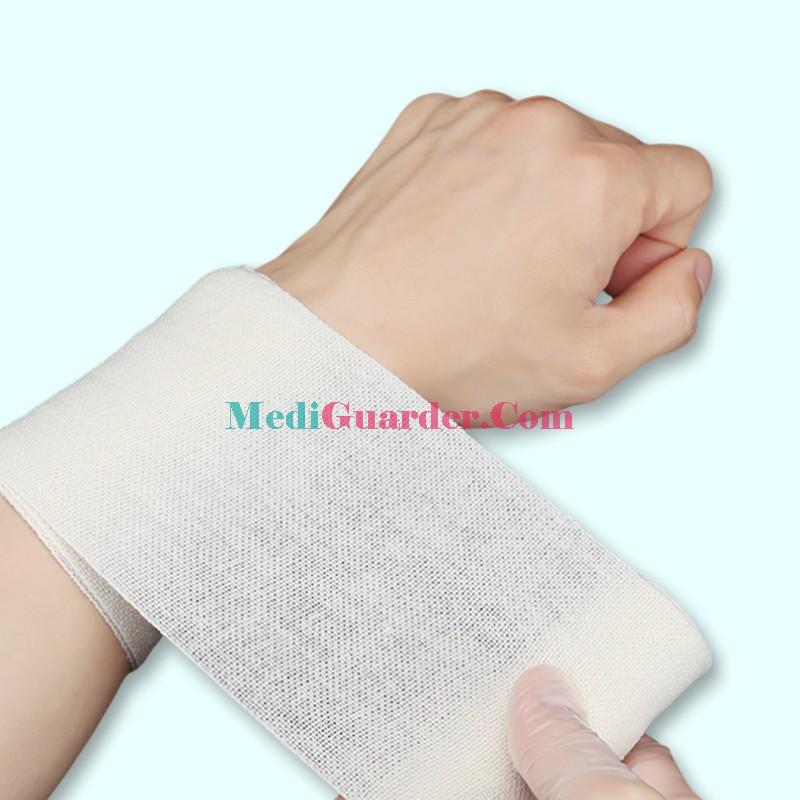
Traditional Passive Dressings
These are the most basic types of dressings, primarily serving to cover wounds and isolate them from the external environment. They do not actively participate in the healing process but rely on the body’s natural healing mechanisms.
Gauze dressings: Made of cotton or cotton-like fibers, they are highly absorbent and breathable. They are often used for clean, low-exudate wounds (e.g., minor cuts or abrasions). However, they may adhere to the wound surface when dry, causing pain during replacement.
Absorbent cotton pads: Thick, soft pads designed to absorb moderate amounts of exudate. They are commonly used in conjunction with gauze to enhance absorption.
Petrolatum gauze: Gauze impregnated with petrolatum (vaseline), which prevents adhesion to the wound and maintains a moist environment. It is suitable for dry wounds, burns, or skin graft sites.
Interactive Dressings
These dressings interact with wound exudate or tissues to actively promote healing. They are widely used in managing acute and chronic wounds with varying exudate levels.
Hydrocolloid dressings: Composed of gelatin, pectin, and carboxymethylcellulose (CMC). They absorb exudate to form a gel-like barrier, maintaining a moist wound environment and promoting autolytic debridement (the natural breakdown of dead tissue). They are ideal for low to moderate exudate wounds, such as pressure ulcers (stage II) or diabetic foot ulcers.
Hydrogel dressings: Water-based or glycerin-based gels that provide moisture to dry, necrotic wounds. They help soften dead tissue and are suitable for burns, radiation-induced wounds, or wounds with little exudate.
Alginate dressings: Derived from seaweed, these dressings form a gel when in contact with exudate, effectively absorbing large amounts of fluid. They are used for heavily exuding wounds, such as venous ulcers or surgical wounds with significant drainage.
Foam dressings: Made of polyurethane foam, they are highly absorbent and provide thermal insulation. They are suitable for moderate to heavy exudate wounds and can be used under compression bandages.
Biological and Advanced Dressings
These dressings are designed to mimic the natural extracellular matrix or deliver active ingredients to accelerate healing.
Collagen dressings: Derived from animal collagen (e.g., bovine or porcine), they promote cell proliferation and tissue repair. They are used for chronic wounds, such as pressure ulcers and venous stasis ulcers.
Silver-containing dressings: Embedded with silver ions, which have broad-spectrum antimicrobial properties. They are effective in preventing and treating infected wounds, such as burns or wounds with signs of bacterial colonization.
Transparent film dressings: Thin, breathable polyurethane films that act as a barrier against water and bacteria while allowing oxygen exchange. They are used for superficial wounds, IV insertion sites, or as a secondary dressing to secure other dressings.
Applications of Medical Dressings
The selection of medical dressings depends on the type, stage, and condition of the wound, as well as the amount of exudate. Here are their main applications:
Acute Wounds
Minor cuts and abrasions: Traditional gauze or transparent film dressings are commonly used to protect the wound from contamination.
Burns: Hydrogel dressings (for superficial burns) or silver-containing dressings (for preventing infection in deeper burns) are preferred. Alginate dressings may be used for burns with significant exudate.
Surgical wounds: Foam dressings or non-adherent gauze are often used to absorb drainage and protect the incision site, reducing the risk of infection.
Chronic Wounds
Pressure ulcers: Hydrocolloid or foam dressings are suitable for early-stage ulcers, while alginate or collagen dressings may be used for more advanced stages with exudate or necrotic tissue.
Venous ulcers: Compression therapy combined with foam or alginate dressings (to manage exudate) is a standard approach.
Diabetic foot ulcers: Silver-containing dressings (to prevent infection) and collagen dressings (to promote healing) are commonly used, along with off-loading devices to reduce pressure.
Special Wounds
Infected wounds: Silver-containing dressings or antimicrobial-impregnated gauze help control bacterial growth. Dry, necrotic wounds: Hydrogel dressings moisten the tissue, facilitating debridement.
Usage Methods of Medical Dressings
Proper application of medical dressings is critical to ensuring their effectiveness and preventing complications. The general steps are as follows:
Preparation
Wash hands: Use soap and water or an alcohol-based hand sanitizer to prevent cross-contamination.
Gather supplies: Prepare the chosen dressing, sterile gloves, saline solution (for cleaning), and scissors (if needed).
Assess the wound: Check the size, depth, exudate amount, and presence of infection (e.g., redness, pus, or odor) to confirm the appropriate dressing type.
Wound Cleaning
Gently clean the wound with sterile saline or a wound cleanser to remove debris and exudate. Avoid using harsh antiseptics (e.g., hydrogen peroxide) as they may damage healthy tissue.
Pat the surrounding skin dry with a sterile gauze pad to ensure the dressing adheres properly.
Dressing Application
For non-adherent dressings (e.g., petrolatum gauze): Place the dressing directly on the wound surface, ensuring full coverage. Secure with a secondary dressing (e.g., tape or a bandage) if necessary.
For hydrocolloid or foam dressings: Remove the backing and apply the dressing to the wound, pressing gently to ensure adhesion. Avoid stretching the dressing, as this may cause skin irritation.
For alginate dressings: Cut the dressing to fit the wound size and pack it lightly into the wound cavity (if applicable). Cover with a secondary dressing to contain exudate.
Securing and Monitoring
Secure the dressing with medical tape, bandages, or a wrap, ensuring it is snug but not too tight (to avoid restricting blood flow).
Document the dressing change, including the wound condition and any observations (e.g., exudate color or odor).
Follow the recommended dressing change frequency (varies by type: hydrocolloid dressings may last 3–7 days, while alginate dressings may need daily changes for heavily exuding wounds).
Removal
Remove the dressing gently to avoid damaging new tissue. For adhesive dressings, peel from the edges toward the center. If the dressing is stuck, moisten it with saline to ease removal.
Conclusion
Medical dressings are vital tools in wound care, with a wide range of types designed to address diverse wound needs. Understanding their classification, applications, and proper usage methods ensures optimal wound healing and reduces the risk of complications. Healthcare providers and patients should collaborate to select the most suitable dressing based on individual wound characteristics, ensuring effective and safe care.
 China Disposable Medical Supplies, Medical Consumables Supplier
China Disposable Medical Supplies, Medical Consumables Supplier
WhatsApp
Scan the QR Code to start a WhatsApp chat with us.